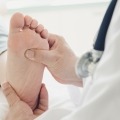
How Diabetes Impacts You Mentally Just as Much as Physically
By Shawn Laib
 A diabetes diagnosis can be frightening and confusing. Taking care of your mental health (as well as your physical health) is key to living a healthy life with diabetes. Shawn Laib discusses his journey coming to terms with his diagnosis and what he has learned from others.
A diabetes diagnosis can be frightening and confusing. Taking care of your mental health (as well as your physical health) is key to living a healthy life with diabetes. Shawn Laib discusses his journey coming to terms with his diagnosis and what he has learned from others.
When I was diagnosed with type 2 diabetes in the spring of 2020, my mind was running a million miles a minute with morbid questions and gut-wrenching anxiety. I was only 24 years old, so my immediate thoughts ran the typical gamut that you would expect from such a startling revelation, including:
-
“Am I going to die at 50 now?”
-
“I love eating pasta, rice, cookies, and cakes, so does this mean these carb-loaded treats are completely off-limits?”
-
“Did I do something wrong, and how could I have avoided this fate?”
I sat in my bedroom and cried for hours at the impending events I imagined would now quickly approach. It’s hard to think of many other times I’ve felt so alone.
Diabetes is a chronic disease, so you have to cope with the reality that there is no “cure” at this moment – you must conform to the best available knowledge about managing your glucose and making smart lifestyle changes. I don’t have to take insulin yet, but it is something I think about having to prepare for every time I go in for my A1C check.
Diabetes attacks virtually every organ in the body, I have learned, and the physical effects can be serious. From nerve damage and glaucoma, to urinary tract infections and increased risk of heart disease, these are scary propositions that people newly diagnosed with diabetes have to come to terms with. It’s a lot to take in, and many newbies don’t also appreciate at first the hefty mental health toll it can take as well.
Diabetes researchers Richard I. G. Holt (University of Southampton, UK), Mary de Groot, (Department of Medicine and the Diabetes Translational Research Center, Indiana University), and Sherita Hill Golden (Johns Hopkins University Schools of Medicine and Public Health) found that diabetes and depression occur together twice as often as comorbidities than they do on their own as separate health problems.
Which one causes the other can be tricky to pin down because both conditions feed into each other. Depression causes poor sleeping habits, unhealthy dietary choices, and a lack of physical exercise. All of these things are risk factors for type 2 diabetes. When you combine the two conditions, each one gets worse.
I know from experience, this can snowball negatively, and finding a way out of the diabetes and depression tag team can be tough. Finding a way to make positive changes can save your life. For me, when I found that 5 mg of glipizide and moderate exercise several times a week lowered my A1C to under 7.0%, it flooded me with relief and euphoria. I knew that I was no longer tied to my chronic illness, that I would not be defined by my problem. It made me try even harder to eat better and take initiative to be healthy, forming that same bidirectional relationship referenced above between mental and physical health.
[Editor’s note: Glipizide is a type of glucose-lowering medication called a sulfonylurea (or SFU) that can lead to severe hypoglycemia. To learn more about SFUs and the risks they pose, click here; to learn more about hypoglycemia, click here; to learn about other medication options such as metformin, DPP-4 inhibitors, SGLT-2 inhibitors, and GLP-1 receptor agonists, check out our medication resource page here.]
My story is just one version of the many-pronged mental health monster that is diabetes. Thomas Larsen is a social studies teacher at Kentwood High School, where I went to school, in Covington, Washington. He was diagnosed with type 1 diabetes when he was 13 years old after his mother was worried about a sudden weight loss of nearly 20 pounds in 10 days. I went to him for advice about how to handle my diagnosis.
“How you start out with diabetes plays a huge role in your mental health throughout your life thereafter,” Larsen told me. “The shock and panic of a diagnosis hits you over the head. You have to be constantly aware of blood sugars, insulin levels, how you're feeling. You have to anticipate when and what meals and activity will be to determine insulin doses. If you're wrong, you could end up in an ambulance or a coma.”
Too many parents and patients have their lives turned upside down with the diagnosis and thereafter live in a state of constant panic.
“I see it constantly in my students who have type 1,” Larsen said. “Most let the disease control them, rather than them controlling the disease and just living life. It adds up. Transitioning over the years from two shots a day to five or more shots a day to an insulin pump all were mentally exhausting because you have to constantly be anticipating, adjusting, and sometimes limiting what you are willing to do.”
I appreciated how Larsen explained ways to overcome mental health challenges while accepting that diabetes is a part of your life. He is 47 years old and has coped with mood swings, failed relationships, and aborted plans to live in foreign countries due to his diabetes. Still, he has been able to manage his blood sugar and has adapted.
Another person I turned to for advice was Dave Raftis, a friend who lives in Kent, Washington. He has lived with a chronic condition called nephrogenic diabetes insipidus since early childhood [Editor’s note: nephrogenic diabetes insipidus is a rare disorder of the kidneys in which they cannot reabsorb fluids normally or healthily. It has no connection to either type 1 nor type 2 diabetes mellitus].
Dehydration and excessive trips to the bathroom caused by his condition are a constant source of anxiety and depression for him. Though our conditions are vastly different, I have learned a lot from him on how to overcome the mental challenges of living each day with a chronic condition.
“From my earliest memories, I was in and out of hospitals for experiments, tests, and regular monthly check-ups with my genetics defect specialist,” Raftis told me. “In school I was treated differently because I had to eat a special diet and had to be allowed to use the bathroom every hour. It brought unwanted attention upon myself which made me extremely self-conscious.”
“I suffered from a lack of confidence and still to this day find myself from time to time not believing in myself,” Raftis said. “Starting at an early age, sports gave me an outlet to overcome my mental challenges. Even today, I stay active and challenge my body and mind with cycling, running, triathlons, etc. I surround myself with like-minded people and manage to push my self-doubt, depression, and anxiety out.”
I find these men inspiring, showing the possibility of overcoming life’s challenges and struggles. Once the physical part of diabetes is managed, accepting yourself for who you are and not letting it interfere with your mindset is just as crucial.
Never let anyone tell you that diabetes defines you. If you are struggling with chronic depression and anxiety from diabetes, contact a mental health professional. For more information on addressing mental health with diabetes check out some of diaTribe’s articles on the subject:
-
How to Find Experienced Mental Health Care Providers for People with Diabetes
-
How and Where to Find In-Person Support Groups and Social Activities for Young Adults with Diabetes
 About Shawn Laib
About Shawn Laib
Shawn Laib graduated from the University of Washington Class in 2020 with a degree in English Literature. He is a fan of video games and basketball. He was diagnosed with type 2 diabetes last year. Follow his writings about diabetes, The Sopranos, gaming and whatever else is on his mind on Medium. Twitter: @LaibShawn.